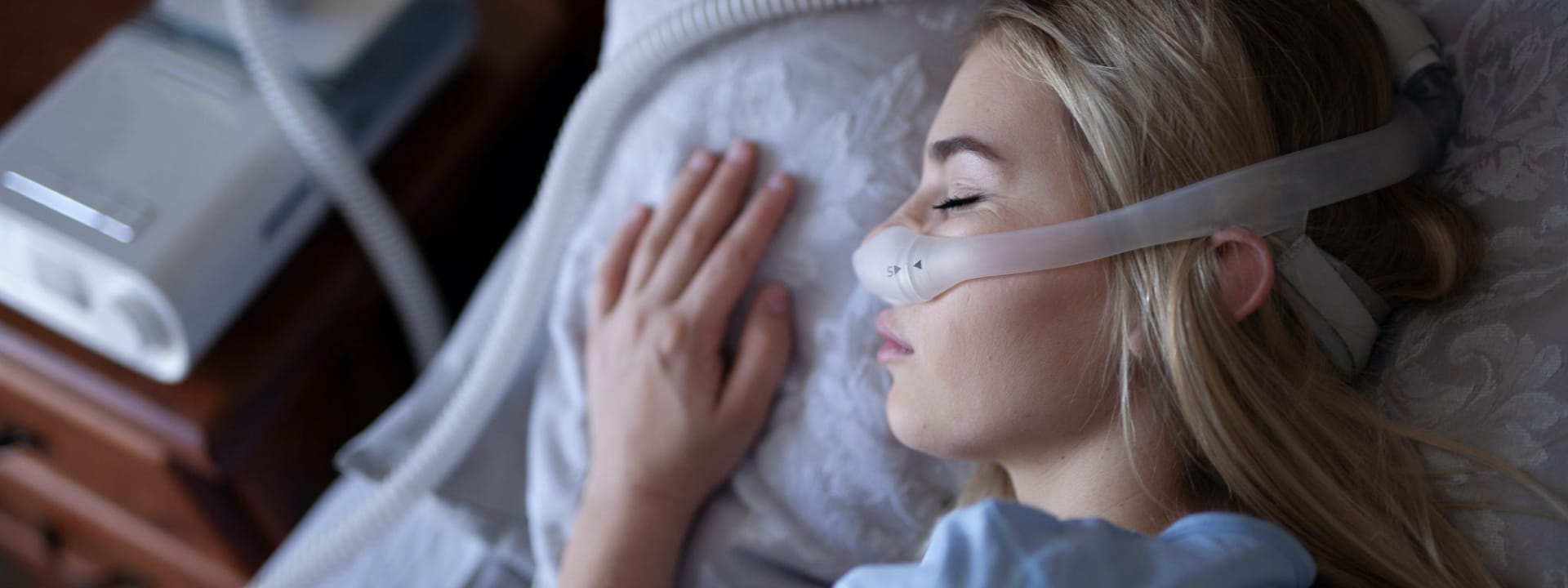
All Party Parliamentary Group for Sleep Apnoea launch
19 February 2024 | Uncategorised

Michael Oko contributes to #SleepAwarenessCampagin2021 in The Guardian
29 April 2021 | Uncategorized

Sleeping Disorders Centre Offers Online Service
7 March 2021 | Uncategorized

No Evidence CPAP Use Increases Coronavirus Risk
7 March 2021 | Uncategorized
Is Sleep Apnoea a Risk Factor for COVID?
7 March 2021 | Uncategorized
Are you holding your breath in your sleep?
11 February 2018 | Uncategorized

3D Scanner Installed at Harley Street Clinic
29 January 2017 | News releases

Michael Oko reviews latest sleep aids for Daily Mail
26 December 2016 | Media

Snore Centre interview wins BJTC award
26 December 2016 | TV and radio
Help Phoebe stand up to her disability
7 September 2016 | Uncategorized

Listen to “Snore and Peace”
28 June 2016 | Uncategorized